Male Stress Incontinence Procedures
JOIN OUR NEWSLETTER
Receive custom tools to help you manage your condition and get the latest in bladder and bowel health from NAFC!
Male Stress Incontinence Procedures
For men with mild to moderate SUI (i.e., relying on fewer than five absorbent pads per day), a male sling procedure is considered a viable treatment alternative. This synthetic mesh provides support so the urinary sphincter can function properly.
ANATOMY
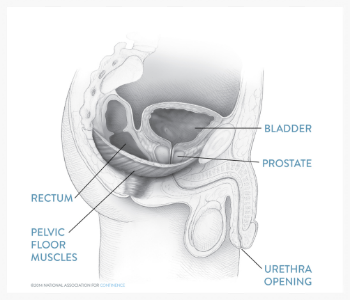
The diagram below gives a simplified view of what’s happening inside a male body. The male sling is surgically implanted around the urethra near the urinary sphincter. The position is key to taking stress off the urinary sphincter in an effort to restore continence.
EVALUATION
Diagnostic tests may be done to evaluate function and the exact cause of the leakage. Your physician will review your medical history and perform a physical exam to get a better sense of your condition and to consider possible treatment strategies.
In particular, he or she may ask you to keep what’s called a ‘bladder diary’ where you detail your urinary habits. Your physician may also request other evaluations, including a urine flow test, blood tests, cystoscopy and urodynamic testing, among others.
SURGERY
The best candidates for a male sling are men with no previous history of pelvic radiation therapy and men who have not had an artificial urinary sphincter implanted. The surgical procedure to implant a sling takes about one hour and can be done either on an outpatient basis or with an overnight hospital stay.
AdVanceTM XP Male Sling System
The AdVance XP Sling is designed to stop leakage by supporting the sphincter muscle. The sling is a strip of soft mesh placed inside the body. The AdVance XP Male Sling moves the sphincter back to its natural position to help restore bladder control. The AdVance XP Sling requires no action by the patient to function. The sling procedure is usually done on an outpatient basis and is performed under anesthesia. Small openings are made to access the urethra and the urinary sphincter. The sling is placed under the urethra and tensioned to reposition the urethra and optimize the sphincter’s function. Most patients are continent immediately following the procedure and can resume normal, non-strenuous activities within a few days. (Learn more.)Coloplast Virtue® Male Sling
A minimally invasive treatment designed for mild or severe SUI in male patients. Combining technologically advanced design, construction, and materials, Virtue® offers a potentially safer, more effective treatment solution than other male slings and possibly artificial urinary sphincters. Virtue® is a permanent solution. Virtue® is the only male sling that utilizes a four-arm approach that uses both elevation and compression to alleviate stress urinary incontinence. A polypropylene mesh material is implanted underneath the bulbous urethra to elevate and apply a gentle compression to prevent urine leakage.
AdVance® Male Sling
A small sling made of synthetic mesh is placed around the urethra through three small incisions. The sling supports the urethra, and possibly partially compresses the urethra. Following the procedure, a catheter may be left in place for 24 hours.
Artificial Urinary Sphincter
For those with moderate to severe SUI, your physician may recommend implementing an artificial urinary sphincter (AUS). In use for more than 25 years, more than 100,000 AUS devices have been successfully implanted in men to treat SUI.
The AUS is implanted into the body to correct stress urinary incontinence in men with significant sphincter damage and thus more severe leakage. The AUS has three components:
- A cuff that helps to close the urethra
- A pump placed inside the scrotum
- A pressure regulating balloon which is placed in the lower abdomen
AMS 800TM Artificial Urinary Sphincter
The AMS 800 System is filled with saline and uses the fluid to open and close the cuff surrounding the urethra. When you need to urinate, you squeeze and release the pump in the scrotum several times to remove fluid from the cuff. When the cuff is empty, urine can flow out of the bladder. The cuff automatically refills in a few minutes squeezing the urethra closed to restore bladder control. The AUS procedure can be performed on an outpatient basis or may require a short hospital stay. Small openings are made near the scrotum and below the abdomen to insert an inflatable cuff, a pump and a small balloon (pressure regulating balloon). The surgery is performed under anesthesia. Four to six weeks after surgery, you will return to the urologist’s office to have the AUS activated. (Learn more.)RECOVERY
The AUS procedure typically takes about an hour to perform and can be done either on an outpatient basis or with an overnight hospital stay. It is important to remember that this is major surgery and one should follow the guidelines set for by the surgeon to get you back on your feet. The following guidelines may be adjusted to meet the specific details of your surgery.
The day after surgery, your catheter will be removed and usually antibiotics are prescribed. Pain medication is offered on an “as needed” basis. While some discomfort is expected, if you experience more pain than you can tolerate, ask for help.
After leaving the hospital, here are some things to expect:
You should continue walking when you return home, gradually increasing the amount of walking you do each day. Short frequent walks of 10-15 minutes are a good starting point (at least 3-4 times per day). Walking will help you rebuild strength.
Take planned rest periods during the day. The best gauge is your body and how you feel.
You may walk up and down stairs as soon as you return home, but take them slowly.
Avoid heavy lifting (greater than 5 pounds) or strenuous activity for 6 weeks after you are discharged. Heavy lifting can increase abdominal pressure, which can put a strain on your incision. If you need to brace yourself to pick something up, then it is too heavy. Five pounds is equivalent to a large telephone book or a gallon of milk.
Avoid bending. This is tiring and also increases abdominal pressure. If you must pick something up, bend with your knees (not at your waist).
Do not resume sexual activity until you discuss it with your doctor at your first postoperative visit. Your doctor will let you know when you can resume sexual activity, typically after 6 weeks.
Do not drive for 4 weeks or as directed by your doctor. A good rule is to not drive until you are pain free. This is because when you are having pain, it will change the way you would react to something. You can be a passenger in the car but on long car trips, take frequent breaks, get out of the car and walk around for a few minutes.
Do not drive any motorized vehicle or sign any documents while taking narcotic pain medication. The narcotic medication may cause changes in visual perception and impair your judgment.
The device can usually be used beginning about 6 weeks after surgery and most men report to be happy with the decision to undergo surgery.
IS SURGERY FOR ME?
The decision to have surgery to treat stress incontinence is often a difficult one. With appropriate evaluation and treatment, problems with SUI are usually treatable so that dignity and quality of life can be restored. Regardless of the treatment option selected, men should continue pelvic muscle exercises to optimize the degree of continence attained and for sexual performance and vitality.
Research indicates that the patient who has only SUI without significant urgency is more likely to be completely satisfied with the results of surgery, but mixed urinary incontinence is not a reason not to undergo surgery.
It all comes down to this: a patient in reasonable health for whom SUI is a significant social problem should seriously consider surgical treatment. The patient should also evaluate the non-surgical alternatives. Most importantly, the patient should feel comfortable asking his physician why a particular procedure is recommended and how much experience the doctor has in performing it.
RELATED ARTICLES

Overactive Bladder in Men
You’ve all probably seen ads on television showing women rushing to the bathroom because of a severe or sudden urge to urinate. That’s overactive bladder

Gender Neutral Pelvic Floor Tips
Simply stated – the pelvic floor isn’t just a female thing – it is a muscular sling supporting the pelvic and abdominal organs of men and women. Here are some great pelvic floor tips for both men and women.

Incontinence During Sex – It Happens To Men Too
Prostate cancer is one of the most common types of cancer in men. According to the American Cancer Society, 1 in 7 men will get

From Postpartum to Postmenopause: The Conversations Women Need to Have
In this episode of Life Without Leaks, we’re joined by Dr. Barbara Frank of Harvard Medical School and Brigham and Women’s Hospital, along with Alex Fennell, co-founder of Attn: Grace, an innovative manufacturer of incontinence products.
Together, we explore the realities of bladder leaks and pelvic floor health during pregnancy, postpartum recovery, perimenopause and menopause, and we discuss why more women are finally beginning to talk more openly about their experiences.
The conversation covers:
• The connection between hormones, menopause and bladder leaks
• Why pelvic floor therapy is having a major moment
• The surprising relationship between pelvic floor tension and incontinence
• How products can impact skin health, comfort and UTIs
• The truth about hormone replacement therapy
• Why community and conversation matter so much in women’s health
Alex also shares the story behind Attn: Grace and the company’s mission to create cleaner, plant-based incontinence products designed to support women with comfort, dignity and confidence.
Whether you’re navigating postpartum recovery, menopause symptoms or simply looking to better understand pelvic health, this episode offers expert insights, practical advice and an encouraging reminder that no one should feel alone in these experiences.




